Thanks to the major advances made in understanding the mechanisms at the root of the disease, today osteoarthritis is no longer considered as simple wear and tear of cartilage. It has now been established that it is under the influence of various risk factors, some of which are modifiable, which makes it possible to envisage the possibility of prevention, at least on an individual scale, in patients at risk.
Why prevent osteoarthritis?
The imperatives are both individual and collective. Osteoarthritis is a chronic condition that develops slowly and is a source of pain which sometimes leads to functional impairment and disablement. While it is not a life-threatening condition, it can have a huge impact on quality of life, be it professional, social or familial.It is a very frequent pathology with considerable economic consequences and its prevalence is regularly increasing in parallel with the ageing of the population.
However, the factors that predict the onset and development of symptomatic osteoarthritis and how it develops are still not very well known. It is difficult at the present time to envisage implementing a primary and secondary prevention policy of the illness on a scale with the population.
How can osteoarthritis be prevented?
Early diagnosis of osteoarthritis is necessary and then choosing a suitable treatment with an aim of relieving the pain, of course, but also of stopping the condition from getting worse, so as to delay the need for surgery for as long as possible and avoid functional impairment and disablement.
To prevent osteoarthritis and its complications, it is essential to fight against the key risk factors which can be summed up as being overweight, joint injury, repeated micro-trauma and various lower limb abnormalities.
How can lower limb abnormalities be corrected?
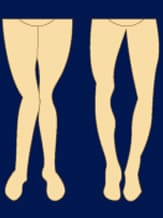
Some lower limb abnormalities can promote the onset of osteoarthritis.
Thus, congenital dysplasia of the hip is a known risk factor of osteoarthritis of the hip.
With regard to the knee, studies have shown that there is more often a valgus deformation in patients with osteoarthritis than in normal patients, without a direct cause and effect relationship being shown. However, we know that these abnormalities promote an increase in osteoarthritis. In practice In non severe osteoarthritis of the knee, without major chondrolysis, with malalignment of the femorotibial joint, osteotomy for valgisation (in the case of knee osteoarthritis on genu varum) or osteotomy for varisation (in the case of knee osteoarthritis on genu valgum) gives good results: it relieves the pain and delays the need for a prosthetic knee joint. Osteotomy for valgisation is most often proximal tibial, involving cutting the upper part of the tibia, removing or adding a bony "wedge" to shift the balance of the tibia towards the outside and thus shift the stress exerted on the damaged medial femorotibial compartment towards the healthy lateral femorotibial compartment. Fixation is generally ensured by staples or a plate and screws.
Osteotomy for varisation, mostly lower femoral, is a delicate procedure.
Which high-risk activities should be advised against?
A relatively mild but regularly repeated traumatism can promote the onset and worsening of osteoarthritis. Hence, carrying heavy loads, working in a crouched or kneeling position or even using power tools such as pneumatic drills or chisels on a frequent basis promotes the onset of osteoarthritis of the spine, knee, elbow and hip.
Another typical example is that of the dressmaker whose frequent use of single finger ring scissors is statistically linked to the development of osteoarthritis of the base of thumb. In the same way, some top-level sportsmen or women who put a lot of strain on their joints develop osteoarthritis more easily: osteoarthritis of the hip in footballers, rugby players and dancers, osteoarthritis of the elbow in javelin throwers, osteoarthritis of the feet in dancers, osteoarthritis of the fingers in judokas.
In practice
Professional activities which provoke or maintain pain must be temporarily or definitively stopped and, in some cases, a job reclassification is necessary (see the article on Osteoarthritis and work).
You need to warn patients at risk of getting osteoarthritis against practising a sport in an intensive and prolonged way!
You need to advise patients with osteoarthritis to take moderate and regular exercise.
In the event of osteoarthritis of the hip and/or knee, they can pursue sports activities that do not require sudden effort such as swimming, cycling or even jogging on condition of doing it on loose soil and with good quality running shoes. Any sport that makes joint pain worse or leads to synovial effusion should be avoided!
Why must any joint injury be treated quickly and efficiently?
A serious joint traumatism responsible for injury to the cartilage is likely to lead to the future onset of osteoarthritis. This is the case, for example, in the classic “dashboard injury” which is sometimes responsible for injury to the cartilaginous menisci of the patella, but also a fracture of the upper part of the tibia sometimes leads to osteoarthritis of the knee, as well as a fracture to the lower end of the leg bone which can lead to secondary osteoarthritis of the ankle.
In the same way, a severe traumatism causing injury close to the cartilage can lead to the future onset of osteoarthritis. This is notably the case for a serious knee sprain (affecting the cruciate ligaments of the knee) or ankle sprain, but also for a tear and, in particular, a meniscal ablation.
This risk is even higher if the meniscus is completely removed and the patient suffers from abnormalities in alignment of the lower limbs and in particular genu varum (bowed legs).
In this case, any intensive high-risk sports activity should be avoided!
Does losing weight really limit the risk of osteoarthritis?
It has now been established that obesity is a high-risk factor in the onset and structural progression of osteoarthritis of the knee (see our article on Osteoarthritis and weight).
A BMI of 30 multiplies the risk of osteoarthritis of the knee by 8
A BMI > 36 multiplies the risk of osteoarthritis of the knee by 13
With a BMI greater than 27, the risk of osteoarthritis of the knee rises by 14% with each increase in kg/m2 of weight! In obese patients there is an increase in mechanical stress to the knee joint. Stress from repeatedly overloading the joints leads to activation of the mechanoreceptors present on the surface of the chondrocytes (integrins, CD44, stretch activated channels). A series of intracellular signalling channels - of which that of NFkB - are thus activated leading to an increase in the expression of IL1 type inflammatory mediators.
The link between obesity and osteoarthritis of the hip has also been established even if it is less apparent than for osteoarthritis of the knee.
One can also observe an increase in the prevalence of nodal osteoarthritis of the hands in obese patients with a relative risk of 1.9. This is difficult to explain by the mechanical overloading factors but suggests the involvement of systemic factors.
Hence, the fatty tissue releases certain pro-inflammatory and anti-inflammatory mediators, the adipocytokines or adipokines, which play a role in the glucidic and lipidic metabolisms. Some of these cytokines of which leptin, adiponectin, visfatin and resistin may also be involved in osteoarthritis.
In addition, diabetes, a frequent comorbidity of obesity, is accompanied by an accumulation of glycation products (AGEs) which may damage the cartilage while stimulating the production inflammatory mediators by the chondrocytes. In practice Even a moderate amount of weight loss of around 5 to 6% of the total weight, enables relieving pain and improving the functional capacities of the overweight patient suffering from osteoarthritis.
Should vitamins be prescribed?
A balanced supply of vitamins C, D and E is recommended through a balanced diet, but at the moment there is no scientific proof to back-up that a dietary supplement (with tablets) is beneficial to osteoarthritis.
Is hormonal treatment indicated?
Osteoarthritis of the knee appears more frequently in women after the menopause than in men.
The cause: the drop in oestrogenic hormone levels, which speeds up the deterioration of the cartilage. Hormonal replacement therapy prescribed, in the absence of any contraindication, to prevent osteoporosis may also contribute to preventing the onset of osteoarthritis. It would appear that osteoarthritis of the hip is observed less frequently in women who have received or are receiving hormone replacement therapy.
In the event of existing osteoarthritis there is no scientific argument to believe that such a treatment could have an effect on its progression.
In all cases, secondaryprevention of osteoarthritis relies on a suitable treatment programme for each patient, according to the severity of their pain, their functional disability, the consequences of their illness on their everyday life, their expectations and their potential.
References:
- Messier SP, Loeser RF, Miller GD, et al. Exercise and dietary weight loss in overweight and obese older adults with knee osteoarthritis: the Arthritis, Diet, and Activity Promotion Trial. Arthritis Rheum 2004;50:1501-10.
- Berenbaum B, Sellam J. Obesity and osteoarthritis: what are the links ? Revue du Rhumatisme 2008; 75: 937-38.
- Christensen R, Bartels EM, Astrup A et al. Effect of weight reduction in obese patients diagnosed with knee osteoarthtitis: a systematic review and meta-analysis. Ann Rheum Dis 2007; 66: 433-9.
- Yusuf E, Nelissen RG, Ioan-Facsinay A et al. Association between weight or body mass index and hand osteoarthritis: a systematic review. Ann Rheum Dis published online 31 May 2009; doi:10.1136/ard.2008.106930.
- Englund M, Guermazi A, Roemer F W et al. Meniscal tear in knees without surgery and the development of radiographic osteoarthritis among middle aged and ederly persons. The Multicenter Osteoarthritis study. Arthritis and Rheumatism 2009; 60 (3): 831-39.









