Several non-pharmacological treatments have a significant symptomatic benefit in osteoarthritis.
All non-pharmacological measures are designed to control pain, reduce joint stiffness, limit damage to the cartilage and improve functioning and quality of life.
Patient education

This requires collaboration between physicians, surgeons, physiotherapists and nutritionists.
One must insist on combating vicious attitudes, going easy on joints, reducing weight and maintaining muscle tone. To improve adherence to the treatment, the physician must explain the expected effects such as decreased pain and increased muscle strength.
The patient must be made aware that stopping a treatment leads to a degradation of the results obtained. They must understand that they need to adopt a new lifestyle.
Resting joints

Going easy on the osteoarthritic joint is recommended. The patient should not "force" a joint during the most painful periods. Resting joints is necessary during flare-ups, but it should not be continued outside of these episodes.
A reasonable amount of regular exercise is advisable to maintain muscle strength.
To improve compliance, measures should be undertaken by the physician, such as regular monitoring and telephone contact with the patient. The patient must actively participate in their treatment and not be passive about it. He or she should be advised to keep a diary with self-evaluation of any progress they notice.
Fighting against being overweight and obesity

There is a significant connection between the body mass index and the risk of developing knee osteoarthritis. Weight loss reduces pain and improves joint function. Being overweight only slightly increases the risk of hip osteoarthritis but when the patient suffers from the latter, the fact of being overweight increases the risk of having recourse to hip replacement surgery.
In addition, digital osteoarthritis is more common in obese subjects.
Weight loss in obese or overweight patients is essential (especially for lower limb osteoarthritic locations). Support from a dietitian may be necessary.
Rehabilitation and exercise

Rehabilitation fights against the formation of a joint deformity by reducing periarticular muscular atrophy and maintaining good joint function. Rehabilitation must be adapted to the patient's pain. It has an analgesic effect and also helps fight against excess weight. This rehabilitation must be regular. It can include muscle-building programmes, maintenance of joint mobility, and stretching and pool exercises (balneotherapy).
During painful flare-ups one must focus on physical activity programmes involving negative pressure or partial pressure on the joints (balneotherapy). Once the rehabilitation exercises with a physiotherapist have been learnt by the patient, they should be continued at home for self-rehabilitation.
Assistive aids

Sometimes auxiliary aids may be indicated. Although it has not yet been proven, their usefulness is recognized by professional consensus. A cane (held in the hand opposite the painful joint) or crutches or even a walking frame for bilateral impairment of the lower limbs, can reduce the pressure on weight-bearing joints and alter the mechanical stress on the damaged joint and thus relieve pain and make walking easier.
Joint braces and splints

The use of braces or splints to rest joints, especially in osteoarthritis of the upper limbs, appears to be effective and is recommended. Their role is to stabilize the joint in a functional position. Ideally, the brace should be custom made. It can be worn continuously during painful episodes or just at night in between flare-ups.
Function orthotics can be used during activities.
For locations in the lower limbs, the effectiveness of orthotics has not yet been proven. However, their use is recommended by EULAR (European League Against Rheumatism) and ACR (American College of Rheumatology) in the treatment of knee osteoarthritis. They are designed to correct a deformity and improve function, quality of life and walking. Flexible non-adhesive orthotics, such as elastic knee supports in osteoarthritis of the knee, may have an analgesic effect and reduce the risk of falls in patients with instability and are recommended by OARSI (Osteoarthritis Research Society International).
Footwear and foot orthotics
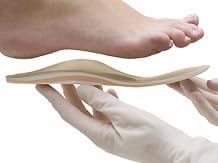
Adaptation of footwear is required in case of impairment of the lower limbs. Orthopaedic shoes and/or shock-absorbing insoles can ease the pressure exerted on the joints of the lower limbs and absorb shocks.
Physiotherapy
Thermotherapy (application of heat or cold), massage, ultrasound and physiotherapy have no lasting effect on pain and stiffness but can help with rehabilitation temporarily relieving patients. Recent meta-analyses have concluded, in the absence of proof, of the effectiveness (or ineffectiveness) of such treatments which are, however, recommended by learned societies in the treatment of osteoarthritis of a lower limb and digital osteoarthritis.
Alternative methods
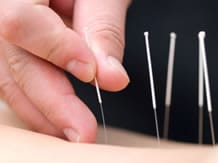
Acupuncture has been evaluated in knee osteoarthritis and appears superior to a placebo in terms of pain relief, while only having a modest effect.
Transcutaneous electrical nerve stimulation can be used, especially after a knee replacement, in order to improve the muscular strength of the quadriceps and help improve function. On non-operated osteoarthritic knees it can have an analgesic effect in the short term.
Bibliography
Stevens-Lapsley et al. Early Neuromuscular Electrical Stimulation Improves Strength and Functional Performance After Total Knee Arthroplasty. ACR 2009 - Philadelphie - 16-21 octobre 2009
Manheimer et al. Acupuncture for peripheral joint osteoarthritis. Cochrane database of systematic reviews 2010.
Rutjes et al. Therapeutic ultrasound for osteoarthritis of the knee or hip. Cochrane database of systemic reviews 2010.
Zhang W et al. EULAR evidence based recommendations for the management of hip osteoarthritis: report of a task force of the EULAR standing committee for international clinical studies including therapeutics (ESCI-SIT). Ann Rheum Dis 2005; 64: 669-8.
Zhang W et al. EULAR evidence based recommendations for the management of hand osteoarthritis: report of a task force of the EULAR standing committee for international clinical studies including therapeutics (ESCI-SIT). Ann Rheum Dis 2007; 66: 377-8.
Jordan KM et al. EULAR recommendation 2003: an evidence based approach to the management of knee osteoarthritis: report of a task force of the standing committee for international clinical studies including therapeutics ( ESCI-SIT). Ann Rheum Dis 2003; 62: 1145-5.
Zhang W et al. OARSI recommendations for the management of hip and knee osteoarthritis, part I: critical appraisal of existing treatment guidelines and systematic review of current research evidence. Osteoarthritis Cartilage 2007; 15(9): 981-1000.
Zhang W et al. OARSI recommendations for the management of hip and knee osteoarthritis, Part II: OARSI evidence-based, expert consensus guidelines. Osteoarthritis Cartilage 2008; 16(2): 137-62.
Zhang W et al. OARSI recommendations for the management of hip and knee osteoarthritis Part III: changes in evidence following systematic cumulative update of research published through January 2009. Osteoarthritis Cartilage 2010; 18: 476-499.
Wang SY, Olson-Kellogg B, Shamliyan TA, Choi JY, Ramakrishnan R, Kane RL. Physical therapy interventions for knee pain secondary to osteoarthritis: a systematic review. Ann Intern Med. 2012 Nov 6;157(9):632-44.










