The treatment has several objectives:
- provide pain relief,
- maintain joint mobility,
- fight against deformities,
- where possible stop joint destruction.
It is based, as for all osteoarthritic locations, on a combination of non-pharmacological and pharmacological treatments. Patient education is an integral part of the treatment: if the patient better understand their illness, their compliance is better. The patient must actively participate in their treatment.
This management is multidisciplinary involving a general practitioner, rheumatologist, orthopaedist, occupational therapist, physiotherapist, dietitian and psychologist (it is not uncommon to see a depressive syndrome in these patients whose disease sometimes has a heavy impact on their quality of life).
Non-pharmacological treatments
Rehabilitation
Exercises have a positive effect on symptoms and function. They promote independence and improve quality of life.
To be effective, they must be done regularly. Compliance will be better if the patient keeps a daily diary and is regularly monitored. Recommendations even mention the need for regular telephone contact with the patient. Physical activity should be recommended outside of flare-ups and adapted to the patient. The exercises are planned and taught by a physiotherapist or in a rehabilitation centre and then put into practice at home.

Lifestyle
The patient must understand and accept the principle of going easy on their joints. They must adapt their environment and way of life based on their physical potential, adapting pace of rest and work according to their joint fatigue. Assistive aids such as canes can help by enabling negative weight therapy. It should be held on the opposite side to the diseased hip. In case of bilateral impairment a walking frame could be useful. Sport can be advised by favouring those that do not involve twisting, such as swimming or cycling. Walking and hiking are not contraindicated.
Weight loss diet in case of excess weight or obesity
In the treatment of knee osteoarthritis, weight loss improves function. In hip osteoarthritis, the connection is less obvious and the benefit of weight loss on the symptoms of patients with hip osteoarthritis has not been established. However, by analogy with knee osteoarthritis, common sense suggests that since weight loss is effective in knee osteoarthritis, it may be so in hip osteoarthritis.
General pharmacological treatments
Analgesics, NSAIDs
The efficacy, good tolerance and low cost of paracetamol makes it the first-line analgesic. It can be prescribed up to 4 g per day except in cases of renal insufficiency or chronic alcoholism, where is limited to 3 g. If that fails, NSAIDs (if necessary with gastric protection) or a coxib may be proposed, by limiting their prescription to the shortest possible period of time.
Symptomatic slow-acting drugs in osteoarthritis
In several studies regarding hip osteoarthritis, SYSADOAs showed efficacy on pain and functional disability. They work after a period of several weeks.
Intra-articular pharmacological treatments
Corticosteroid injections
This type of injection can quickly relieve the painful joint during an acute flare-up of osteoarthritis. For this deep joint, it is necessary to carry out the injection under visual control (scopy or ultrasound).
Surgical treatment
Preventive
Preventive conservative surgery is for young patients and aims at slowing down the osteoarthritic process.
Several techniques are used:
- in case of an axis defect, a femoral osteotomy may be considered.
- in case of hip dysplasia (insufficient coverage of the femoral head by the roof of the acetabulum), acetabular surgery with the fitting of an preventive abutment is proposed. The goal of this surgery is to increase the size of the acetabulum and thus change the force exerted on the hip.
A preventive action can also be offered in case of anterior femoro-acetabular impingement.
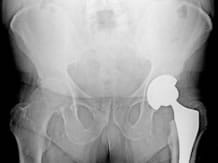
Curative
This involves total hip replacement. It is necessary to ensure that the medical treatment has been correctly implemented before offering the patient hip replacement surgery.
The patient's functional impairment must be evaluated. Certain functional tests (Lequesne's test for example) to quantify this discomfort and guide the indication of a prosthesis.
It is recommended to prescribe pre-operative rehabilitation which should include physiotherapy and offer therapeutic patient education to the patient.
Post-operatively, rehabilitation sessions are prescribed on an outpatient basis when the patient returns home. For patients with impaired function, associated comorbidity or complications from surgery, the completion of the rehabilitation is conducted in the appropriate facilities.
Special case of rapidly destructive hip osteoarthritis
Negative pressure therapy is particularly indicated, combined with a treatment of intra-articular corticosteroid injections. In most cases, unfortunately, the evolution leads to substantial joint destruction requiring total hip replacement.
Bibliography
- Le Coniat Y and coll. Traitement chirurgical de l’arthrose des membres. Réalités en rhumatologie avril 2008, N°6.
- Roddy E and coll. Evidence –based recommendations for the role of exercise in the management of osteoarthritis of the hip or knee. The move consensus. Rheumatology 2005; 44 : 67-7.
- Zhang W and coll. EULAR evidence-based recommendations for the management of hip osteoarthritis: report of a task force of the EULAR standing committee for international clinical studies including therapeutics (ESCI-SIT). Ann Rheum Dis 2005; 64 : 669-8.
- Zhang W and coll. OARSI recommendations for the management of hip and knee osteoarthritis, part I: critical appraisal of existing treatment guidelines and systematic review of current research evidence. Osteoarthritis Cartilage. 2007; 15(9) : 981-100.
- Zhang W and coll. OARSI recommendations for the management of hip and knee osteoarthritis, Part II: OARSI evidence-based expert consensus guidelines. Osteoarthritis Cartilage. 2008; 16(2) : 137-6.
- Zhang W et al. OARSI recommendations for the management of hip and knee osteoarthritis Part III: changes in evidence following systematic cumulative update of research published through January 2009. Osteoarthritis Cartilage 2010; 18: 476-499.