The management of knee osteoarthritis is based on lifestyle changes, physical therapies, oral drug treatments, local treatments and surgery.
Recommendations have been made by several learned societies: EULAR in 2003 and OARSI in 2008. All agree on the importance of non-drug therapies.
The patient must first be empowered and educated. Self-management should be encouraged rather than a passive attitude.
Non-pharmacological treatments
Weight loss
Patients with osteoarthritis who are overweight or obese have an increased risk of worsening of their knee osteoarthritis, or developing the contralateral knee osteoarthritis. It is important to advise an overweight or obese patient to lose weight. It may be necessary to involve a dietician or nutritionist in the patient's care programme.
Exercise
Physical activity improves function and quality of life. One must of course adapt the exercise to the patient's capacities.
Increased physical activity improves the efficiency of a weight loss diet. Indeed, weight loss is related to the amount of exercise.
An exercise programme can be recommended to the patient. They are planned and taught by a physiotherapist, a doctor or physical rehabilitation centre and then put into practice by the patient at home. To be effective, they must be done regularly.
One can, for example, recommend regular walking.
Shoes and insoles
Flexible orthopaedic insoles are shock absorbing and can be of service. In the event of osteoarthritis of the tibiofemoral compartment, insoles with lateral elevation are recommended. High heels of more than 4 cm are not recommended because they promote flexion.
Orthotics and canes
Restraining the knee can range from a simple knee brace to a rigid orthosis. A walking stick (or a simple umbrella) is useful as it enables negative pressure on the joints. The cane should be held on the opposite side to the osteoarthritic joint. This cane is recommended for steps or during flare-ups of the disease for partial negative pressure on the joint.
In case of bilateral knee osteoarthritis, the patient can exchange the stick against a walking frame, possibly with wheels.
Rehabilitative treatment

This treatment has several objectives:
- fight against pain with massages, physiotherapy and balneotherapy enabling working on the joints with negative pressure therapy,
- maintain joint mobility and muscle tone by working on posture and strengthening the quadriceps muscle and also other stabilising muscle groups of the knee,
- prevent vicious attitudes (flexion),
- educate the patient about the benefits of going easy on their joints. Resting the joints is essential in the event of a flare-up. The patient should be advised to avoid carrying heavy loads, prolonged standing, long walks on bumpy ground, going up and down the stairs, squatting and kneeling work.
Systemic treatments
Analgesics: paracetamol
The choice of analgesic treatment is based on a precise estimate of the pain. The severity of pain must be taken into account in order to prescribe a suitably effective analgesic. The recommended first-line analgesic is paracetamol up to 3 grammes per day.
Repeated doses are necessary for good efficacy, which must be explained to the patient. Its tolerance is good. In the event of renal insufficiency or chronic alcoholism, doses should be adjusted accordingly.
Non-steroidal anti-inflammatory drugs and Coxibs
NSAIDs should be reserved for second-line use in the event of failure of the paracetamol and/or in case of an inflammatory flare-up.
They should always be prescribed and used at the lowest effective dose and for the shortest possible time.
The choice of NSAID must be made taking into account its safety profile an the individual risk factors for the patient.
Conventional NSAIDs or Coxibs should not be prescribed in the event of a peptic ulcer or gastrointestinal bleeding, a history of gastrointestinal bleeding or perforation occurring during a treatment with NSAIDs.
NSAIDs being capable of inducing acute renal insufficiency, one must be particularly attentive to patients treated with diuretics, at risk of hypovolemia or impaired renal function.
In patients with known ischemic heart disease, peripheral arterial disease and/or a history of stroke (including transient ischemic attack), coxibs are contraindicated and non-selective anti-inflammatory drugs should be used with caution.
Symptomatic slow-acting drugs in osteoarthritis
In several studies regarding knee and hip osteoarthritis, SYSADOAs showed efficacy on pain and functional disability. They work after a period of several weeks. Some of them have a remnant effect of 1 to 2 months on stopping them and significantly reduce the consumption of NSAIDs.
Opioid analgesics
In cases of unremitting pain, intolerance to paracetamol or contraindications to NSAIDs, it is possible to use level 2 and 3 analgesics of the WHO (weak and strong opioids).
They can enable getting through a period but at the cost of frequent undesirable side effects (nausea and vomiting, disorders of higher functions, severe constipation). Their indication and their risk/benefit ratio must be thoroughly assessed.
Local treatments
Topical treatments
Applied locally, NSAIDs are effective in mild osteoarthritis. They have fewer side effects and better tolerance than oral NSAIDs.
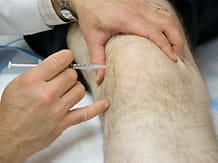
Intra-articular treatments
Analgesic treatments administered in intra-articular injections may also be used.
Corticosteroids
Used as symptomatic treatment for all osteoarthritic joints, they can be injected directly into the painful joint in the event of a painful flare-up to give fast relief to the patient: Their effects usually fade within a few weeks. In osteoarthritis of the knee, corticosteroid injections under "scopic" or ultrasound control is not necessary. Rest of the injected joint is recommended for 24-48 hours after the procedure.
Hyaluronic acid
Hyaluronic acid injections have a delayed analgesic effect whose effect extends over the medium term (3 to 6 months and up to 12 months) in osteoarthritis of the knee and are part of EULAR recommendations for the symptomatic treatment of knee osteoarthritis.
Treatment with hyaluronic acid is indicated in knee osteoarthritis of moderate severity. It consists of three intra-articular injections spaced one week apart. This treatment has a delayed action. Its action lasts for between 6 and 12 months. Single injection treatments have recently been developed showing no difference in efficacy compared to those requiring three injections. This therapeutic effect is significantly greater than that of a placebo. This treatment is well tolerated and has few side effects.
Studies regarding potential structural effects are contradictory and do not currently enable using these molecules with structural effects.
There are many hyaluronic acids (HA) commercialised in France. Their main difference lies in their molecular weight. There is no formal proof of the superiority of high molecular weight HA in relation to low weight.
Surgical treatments
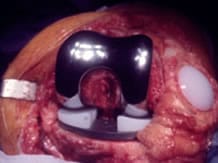
Conservative surgery may be considered in younger patients with an axis defect and unicompartmental osteoarthritis in the early stages. This surgery is based on realignment osteotomy.
Arthroscopic lavage with with arthroscopic debridement is controversial.
It may be necessary to resort to fitting a prosthesis of the knee. For this there has to be a advanced radiological anatomical osteoarthritis, pain and/or major functional disability in spite of a well conducted medical treatment over a sufficient period of time.
Resorting to arthrodesis of the knee is exceptional being reserved for failures or complications of prostheses and patients with a defect of the extensor mechanism.
Bibliography
- Christensen R et al. Weight loss: the treatment of choice for knee osteoarthritis? A randomized trial. Osteoarthritis cartilage 2005; 13 : 20-27.
- Jordan KM et al. EULAR recommendation 2003: an evidence based approach to the management of knee osteoarthritis: report of a task force of the standing committee for international clinical studies including therapeutics (ESCI-SIT). Ann Rheum Dis 2003; 62 : 1145-55
- Zhang W et al. OARSI recommendations for the management of hip and knee osteoarthritis, part I: critical appraisal of existing treatment guidelines and systematic review of current research evidence. Osteoarthritis Cartilage 2007; 15(9) : 981-1000.
- Zhang W et al. OARSI recommendations for the management of hip and knee osteoarthritis, Part II: OARSI evidence-based, expert consensus guidelines. Osteoarthritis Cartilage 2008; 16(2) :137-62. Rappel des règles de bon usage des AINS. AFSSAPS 2006.