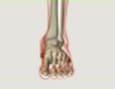
A distinction must be made between patellofemoral osteoarthritis (35% of cases) and femorotibial osteoarthritis.
Patellofemoral osteoarthritis
In patellofemoral osteoarthritis, pain is located in the back of the knee and radiates downwards. It is readily triggered when going up stairs but mostly going down stairs and after prolonged sitting, squatting or kneeling. However, the pain is moderate when walking on level ground. One can find signs of painful jarring, especially when walking, and episodes of effusion, particularly during painful flare-ups.
On examination, pain is awakened:
- on hampered extension of the knee;
- on percussion of the patella on a flexed knee;
- on touching the patella;
- planing manoeuvre (friction of the patella against the trochlea) ;
- Zohlen manoeuvre: pain when the examiner opposes the ascension of the patella during contraction of the quadriceps.
These clinical signs are sometimes difficult to interpret: the knee pain is often diffuse, reflecting the impairment associated with a femoral-tibial compartment.
Femorotibial osteoarthritis
The pain that accompanies femorotibial osteoarthritis is more likely located in the medial compartment (more frequently femoral-tibial internal impairment).
Of the mechanical type, occurring when walking and going up and down stairs, it is relieved by rest, and does not wake the patient up except when changing position.
In an inflammatory flare-up, the pain intensifies, increasing at night with the presence of joint effusion which can sometimes be abundant.
An examination of the knee must be carried out first of all standing, then walking and then lying down.
The examination standing is to look for axial deviations of the lower limbs (genu varum, genu valgum or genu recurvatum).
The examination walking enables showing an increasing impairment of a static nature.
The examination in the supine position examines knee mobility, systematically looks for intra-articular effusion (even in the absence of local inflammatory signs) in the detection of a shock to the patella and tests the anterior-posterior (preserved) and lateral stability of the patella (key element in future indications for surgery).
In advanced osteoarthritis, one can see deformation of the knee, with a globulous appearance and especially a flexion deformity.
Pitfalls to avoid
- A hip disease: normal mobility and the absence of knee pain on palpation and mobilisation should encourage examining the hip and doing and an X-ray of the pelvis
- Metabolic arthropathy: chondrocalcinosis, gout
- Bone disease: tibial plateau fracture, tumour of the acetabulum or femur, femoral and/or tibial Paget's disease, osteonecrosis of the femoral condyle, knee reflex sympathetic dystrophy, etc.
- A non-osteoarticular disease: femoral neuralgia, sural or popliteal phlebitis, femoral arteritis, etc.
- Abarticular pathology: sprained knee, quadriceps or patella tendinitis or tendinitis of the pes anserinus, etc.