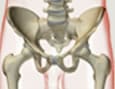
It can affect one or more joints: talonavicular, subtalar, and metatarsophalangeal joint, the most commonly affected.
It occurs most often on a static disorder of the foot or after trauma. The best treatment is prevention: correction of static disorders (wearing corrective insoles) and architectural defects whether acquired or constitutional, prompt treatment of potential fractures.
There are no specific recommendations for its management which do not differ from treatments usually proposed in osteoarthritis and they are therefore based on a combination of non-pharmacological and pharmacological measures.
Non-pharmacological treatments
Orthotic treatment
- Standard orthopaedic shoe models
Good footwear is essential The doctor must stress its importance to the patient. The latter should favour deep and wide shoes. The heel should not be higher than 4 cm. The sole should be thick and of good quality in order to absorb the stresses and shocks.
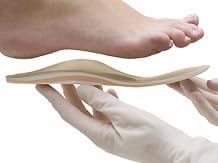
- Foot orthotics
Customised foot orthotics can be made. They should be crafted with precision by a podiatrist, tailored to the patient and can be used in standard shoes provided the heel is no higher than 4 cm. Indeed, over 4 cm, the back of the foot is no longer functional and the front of the foot no longer bends with each step which eliminates the potential action of the insole. It may be necessary sometimes to resort to new shoes half a size bigger in order to get the insole to fit inside.
Foot orthotics are made from flexible materials. They must be adapted to the purpose: distribution of weight, shock absorption, maximum comfort, rigid insole cradling the foot to minimise the movement of the metatarsophalangeal joint in cases of hallux rigidus. The patient should be warned that the orthosis, as with many devices, requires an adjustment period (usually 8-15 days). - Other tailored solutions
In the event of major deformities of the foot in relation to an advanced osteoarthritis, orthopaedic shoes can be made to measure. - Orthotics for toes
Toe orthotics consist in customised devices for toes aimed at reducing a deformity or eliminating a painful pressure point The toe brace is worn when wearing shoes. It can combined with foot orthotics. For example, in the event of a dorsal osteophyte in connection with metatarsophalangeal osteoarthritis of the first ray (hallux rigidus), it reduces the friction with the shoe.
Patient education
It is necessary to inform the patient about the importance of taking measures to go easy on joints. Advice for resting joints must be given. This consists in limiting prolonged periods of standing or walking.
Rehabilitation
Its purpose is to maintain functional potential. It combines several techniques such as walking rehabilitation, foot and plantar massages, stretching exercises, active and passive mobilisation (early hallux rigidus), strength training, proprioception and sensory afferents (stimulate plantar sensitivity) and physiotherapy combining ultrasound and thermotherapy.
Local treatments
They should be favoured over systemic treatments.
Topical treatments
Applied locally, NSAIDs are effective in mild osteoarthritis They have fewer side effects and better tolerance than oral NSAIDs.
Intra-articular corticosteroid treatments
Used as symptomatic treatment for all osteoarthritic joints, they can be injected directly into the painful joint in the event of a painful flare-up to give fast relief to the patient: Their effects usually fade within a few weeks. Rest of the injected joint is recommended for 24-48 hours after the procedure.
Systemic treatments
Analgesics: paracetamol
The choice of analgesic treatment is based on a precise estimate of the pain. The severity of pain must be taken into account in order to prescribe a suitably effective analgesic. The recommended first-line analgesic is paracetamol up to 3 grammes per day.
Repeated doses are necessary for good efficacy, which must be explained to the patient. Its tolerance is good. In the event of renal insufficiency or chronic alcoholism, doses should be adjusted accordingly.
Non-steroidal anti-inflammatory drugs and Coxibs
NSAIDs should be reserved for second-line use in the event of failure of the paracetamol and/or in case of an inflammatory flare-up.
They should always be prescribed and used at the lowest effective dose and for the shortest possible time.
The choice of NSAID must be made taking into account its safety profile an the individual risk factors for the patient.
Conventional NSAIDs or Coxibs should not be prescribed in the event of a peptic ulcer or gastrointestinal bleeding, a history of gastrointestinal bleeding or perforation occurring during a treatment with NSAIDs.
NSAIDs being capable of inducing acute renal insufficiency, one must be particularly attentive to patients treated with diuretics, at risk of hypovolemia or impaired renal function.
In patients with known ischemic heart disease, peripheral arterial disease and/or a history of stroke (including transient ischemic attack), coxibs are contraindicated and non-selective anti-inflammatory drugs should be used with caution after a thorough evaluation.
Opioid analgesics
In cases of unremitting pain, intolerance to paracetamol or contraindications to NSAIDs, it is possible to use level 2 and 3 analgesics of the WHO (weak and strong opioids).
They can enable getting through a period but at the cost of frequent undesirable side effects (nausea and vomiting, disorders of higher functions, severe constipation).
Their indication and their risk/benefit ratio must be thoroughly assessed.
Surgical treatment
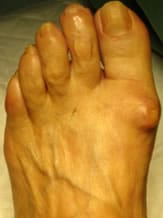
Surgical treatment concerns 90% of cases of hallux rigidus.
It is basically arthrodesis that brings indolence at the cost of loss of mobility usually already largely compromised. Prosthetic replacement of the first metatarsophalangeal joint is controversial. Indeed, the prostheses have all shown a high rate of complications (early aseptic loosening, implant fracture, dislocation, etc.). Outside of the first ray, surgery is proposed as a last resort.
It should be noted that foot surgery is difficult and, depending on the series, complications affect 10 to 30% of cases. The most common complications are infection, blood clots, scarring or unsightly protrusions and the difficulties with footwear (residual oedema).
Bibliography
- Goldcher A. Indications des orthèses plantaires. EMC podologie V 27-130-A-15.
- Mortier JP, Perrier A. Chirurgie des hallux valgus et rigidus. Revue du Podologue 2009 ; 25(30) : 13-15.
- Rappel des règles de bon usage des AINS. AFSSAPS 2006.