Recommendations for the treatment of osteoarthritis of the hand were issued in 2006 by EULAR (European League Against Rheumatism). They concern rhizarthrosis and osteoarthritis of the fingers.
The best treatment combines pharmacological and non-pharmacological methods. However, the choice of treatment remains difficult because of the absence of high quality clinical trials and little proof.
There is a need, before all else, to clarify whether the patient's distress is mainly due to deformity, pain or disability. Individual care and self-management by the patient are vital.
The non-pharmacological treatments, including occupational therapy, physiotherapy, the use of assistive aids (braces or splints) are important in the recommendations.
Non-pharmacological treatments
Rehabilitation
The aim of rehabilitation is to reduce joint stress and maintain joint mobility.
Several techniques are used such as analgesic massage, thermotherapy, ultrasound and exercises. It is important to fight against joint stiffness by rehabilitation because once established, it is irreversible.
The local application of heat (heated dressings, paraffin wax) and ultrasound can provide analgesia for a short period and be provided before exercising.
Occupational therapy
Ergonomic measures should be taken. The patient should be given advice on how to protect their joints. For example, he or she can write with a pen of large diameter and modify fine and fiddly objects that are difficult to grasp, etc.
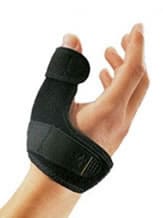
Assistive aids
Splints can prevent stiffness in a bad position, especially in long fingers. Fighting against deformity is also important for the thumb. It needs to be taken care of at an early stage because the progressive deterioration of the joint leads to adductus thumb, loss of mobility and often significant functional impairment. This is compounded by the wasting of the thenar eminence which can be fought against via exercises.
A thumb orthosis stabilises the thumb in a functional position. It has an orthopaedic role against deformity but is also analgesic. It can be worn continuously during acute painful episodes or just at night in between flare-ups when the pain is less disabling.
In practice, custom-made moulded orthotics tailored to the patient enable better adaptation especially if the stiffness is well-established. Good compliance requires good tolerance of the orthosis by the patient.
Pharmacological treatments
Regarding pharmacological treatments, priority should be given to the compound that has the best benefit/risk ratio with regular reassessment of the indication.
Local treatments remain preferable to systemic treatments.
Local treatments
Topical NSAIDs can be used with a good symptomatic effect.
Paracetamol
Paracetamol is the analgesic of choice because it is particularly effective and well tolerated. It can be used up to 3 grammes per day.
NSAIDs and Coxibs taken orally
NSAIDs should be reserved for second-line use in the event of failure of the paracetamol and/or in case of an inflammatory flare-up.
They should always be prescribed and used at the lowest effective dose and for the shortest possible time.
The choice of NSAID must be made taking into account its safety profile an the individual risk factors for the patient.
Conventional NSAIDs or Coxibs should not be prescribed in the event of a peptic ulcer or gastrointestinal bleeding, a history of gastrointestinal bleeding or perforation occurring during a treatment with NSAIDs.
NSAIDs being capable of inducing acute renal insufficiency, one must be particularly attentive to patients treated with diuretics, at risk of hypovolemia or impaired renal function.
In patients with known ischemic heart disease, peripheral arterial disease and/or a history of stroke (including transient ischemic attack), coxibs are contraindicated and non-selective anti-inflammatory drugs should be used with caution.
Corticosteroid injections
During painful flare-ups, intra-articular corticosteroid injections can be offered to patients. They can be radio-guided because access to the joint is often difficult because of the joint space narrowing and osteophytes.
Surgical treatments
In the event of persistent painful symptoms or disability with deformity despite an optimum medical treatment, surgical treatment may be considered.
Bone trimming consists in the resection of osteophytic bone spurs. This procedure does not modify the arthritic development leaving the joint pain and discomfort to persist. This surgery is performed more on a psychological basis.
Digital realignment osteotomy may help in case of misaligned joints that are particularly troublesome.
The aim of arthrodesis consists in joint fusion in a functional position. It provides good pain relief and realigning but causes a loss of mobility.
It can be of interest to distal interphalangeal joints.
Arthroplasties are used for the proximal interphalangeal joints as preserving mobility is essential at this level.
In the particular case of rhizarthrosis, there are 3 surgical options:
- trapeziectomy,
- scaphoid-trapezium arthrodesis,
- trapeziometacarpal prosthesis.
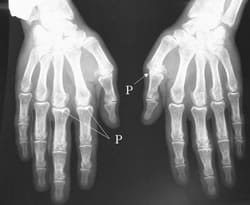
Osteoarthritis secondary to hemochromatosis (joint space narrowing of MCP joints 2 and 3).
CH St. Antoine - Pr. Berenbaum, Dr. Perret and Dr. Villoutreix
Bibliography
- Lellouche H, Roulot E. Prise en charge médico-chirurgicale de la rhizarthrose. Rhumato nov 2008, vol 5, N°42.
- Chabot A. Tout ce qu’il faut savoir sur l’arthrose digitale. Rhumatos mai 2009, vol 6, N°48.
- Zhang W et coll. EULAR evidence based recommendations for the management of hand osteoarthritis: report of a task force of the EULAR standing committee for international clinical studies including therapeutics (ESCI-SIT). Ann Rheum Dis 2007; 66 : 377-88.
- Rappel des règles de bon usage des AINS. AFSSAPS 2006.