Treatment is primarily medical and combines non-pharmacological and pharmacological measures.
Non-pharmacological treatments

Orthotic treatment
During acute flare-ups, wearing a standard or custom-made spinal immobilisation corset has an analgesic effect.
Outside the flare-up episodes, during activities wearing a lumbar support belt (LSB) increases the level of vigilance (avoids potentially painful movements). It should be noted that wearing a LSB, even for prolonged periods of time, involves no risk of muscle loss (abdominal and back muscles).
The "thermal environment" created by the LSB has a muscle relaxant and analgesic action. The LSB has a proprioceptive role. Its psychological impact is not negligible. Patient compliance depends on comfort. A lumbar brace is a brace which effectively allows the patient to be more mobile and exerts an analgesic effect.
Patient education
While no studies prove the effectiveness of a weight loss diet in the lumbar osteoarthritic patient, it is always wise to encourage an overweight or obese patient lose weight. It may be necessary to use the services of a nutritionist or dietitian. As with any chronic illness, compliance depends on the patient understanding their illness and requires the appropriate education.
Rehabilitation, exercises, sport
During acute painful episodes, rest is essential.
Outside the flare-ups, the therapist will give advice on preventive care for the joints and recommend joint physiotherapy exercises with the essential aim of strengthening the abdominal muscles. Regular sports activities suited to the function capabilities of the patient should be recommended and will help maintain a specific weight.
Pharmacological treatments
Analgesics, NSAIDs, muscle relaxants
If long-term medication is necessary, an analgesic treatment such as paracetamol is preferable. Muscle relaxants can also be proposed. In case of failure, especially in the event of an acute painful episode, anti-inflammatory drugs, in combination with gastroprotection or a coxib, may be prescribed respecting the contraindications and for the shortest possible time because of the potential side effects.
Spinal injections
These can be carried out in some instances.
- Indications
Epidural injections have no indication in the lower back pain of lumbar osteoarthritis unless there is an associated radiculopathy.
Posterior zygapophysial joint injections can be given in the event of posterior articular lumbar joint syndrome. They must be performed under radiographic control to ensure their intra-articular character.
If there is symptomatic lumbar spinal stenosis, epidural injections of cortisone derivatives or intradural injections may be offered which then requires a short hospital stay. It should be noted the latter procedure has been abandoned by some teams because of potential complications (cerebral thrombophlebitis).
It has not been proven that these injections in the case of "Lumbar spinal stenosis" reduce the need for surgery, but they often relieve symptoms for a few months. Usually 2-3 epidural injections are performed. - Potential complications
The most common are the worsening of rachialgia and vagal malaise. More rarely, post-lumbar puncture syndrome can occur or an epidural haematoma, nerve damage or infection (epidural abscess, meningitis). - Precautions
Because of possible haemorrhagic complications, this procedure is contraindicated in patients on anticoagulants (AVK). If the injection is necessary, the AVK will be interrupted and relayed by a low molecular weight heparin (LMWH) and performed when the INR is less than 1.5 and 24 hours after the injection of LMWH. If the anticoagulant treatment was prescribed in cardiology, the cardiologists' agreement is necessary before interrupting the treatment.
An epidural injection is not recommended during treatment with an antiplatelet drug. The injection will be carried out ten days after discontinuation of the antiplatelet drug.
Surgical treatment
Example of lumbar spinal stenosis (LSS)
There is little indication of surgery in lumbar osteoarthritis outside of LSS
In the event of LSS type impairment and/or in the event of failure of the medical treatment, surgical treatment may be decided on. However, the medical treatment may be bypassed in favour of early surgery in cases of motor and/or sphincter dysfunction or severe restriction of maximum walking distance.
Its goal is to make the spinal canal diameter sufficient to remove any source of radicular conflict. Recalibration of the lumbar canal is the procedure most often performed (enlargement of stenotic levels). This procedure gives good results. In cases where a destabilization of the spine is feared after surgery, it may be useful to associate arthrodesis of the levels operated on.
Complications of spinal surgery
Complications of lumbar recalibration surgery are rare. However, there are potential neurological complications. They may be the result of direct trauma to the nerve roots or the establishment of a postoperative compressive intraductal haematoma. Dura mater breach or spinal fluid leakage is the most common perioperative incident.
Other complications are those related to any surgery such as phlebitis, embolism and infection. In the long term destabilisation of the spine can occur if an arthrodesis has not been done.
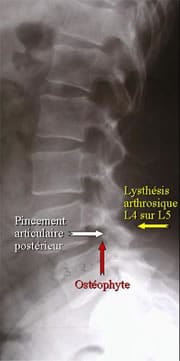
Canal lombaire rétrécis par arthrose articulaire postérieure, rachis lombaire de profil.
CHU Pitié-Salpétrière
Pr. Bourgeois et Dr E.Zinc
Bibliography
- Guigui P. Techniques chirurgicales – Encyclopédie Médico-Chirurgicale Orthopédie-Traumatologie [44-181] 2006 F.
- Lipo et al. La prise en charge thérapeutique de l'arthrose en ce début de 3e millénaire. La revue de médecine interne 2003 ; 24(4) : 243-252.